The Medical Society of the State of New York (MSSNY) represents tens of thousands of physicians, residents, and medical students who provide care across every region of the state, from small private practices and large group settings to hospital employment and public health service roles. Our diverse membership shares a common goal: to ensure that every New Yorker has access to high-quality, affordable, physician-led healthcare.
However, the ability of physicians to deliver this care is increasingly challenged by a growing encroachment into medical decision-making from non-physician providers, health insurers, corporate pharmacy chains, private equity firms, dominant health systems, electronic health record vendors, and policymakers. While these entities may pursue well-intentioned goals of improving care or reducing costs, their actions often limit treatment options, weaken physicians’ ability to advocate for their patients, and drive many doctors out of clinical practice, whether through early retirement, relocation out of state, or displacement by non-physician practitioners.
The Rising Toll on the Physician Workforce
These pressures are taking a measurable toll on physicians’ well-being. A 2025 national survey found that physicians continue to face mounting challenges contributing to burnout, stigma, and barriers to accessing mental health care. The survey higlighted the profound effects of ongoing healthcare consolidation, evolving payment models, the spread of medical misinformation, and significant federal policy shifts. Among the findings:
- 57% of physicians reported experiencing inappropriate anger, tearfulness, or anxiety.
- 46% withdrew from family, friends, or colleagues.
- 55% felt levels of debilitating stress.
- 54% reported frequent feelings of burnout.
- 73% cited stigma surrounding their personal access to mental health care.
These findings underscore an urgent need for systemic reform to protect physicians’ mental health and preserve a sustainable, compassionate workforce capable of meeting New Yorkers’ healthcare needs.
New Policy Threats to Patient Coverage and Access
Physicians’ ability to care for their patients may be further strained by new state-level challenges stemming from recently enacted federal legislation. These changes could cause many patients to lose coverage through essential public health insurance programs such as the Child Health Insurance Program (CHIP), the Essential Plan, and Medicaid.
The new federal law also reduces New York’s capacity to access certain federal funding streams that have long supported these programs. Without these funds, policymakers may struggle to maintain adequate reimbursement for physicians and other healthcare providers, jeopardizing their ability to cover practice expenses, staff salaries, and overhead costs.
In many community-based practices, particularly those serving rural and urban underserved regions, a large share of patients may be covered under these public programs. A significant loss of insured patients could therefore become the final blow for already struggling practices. The New York State Comptroller’s Office has warned that many rural counties already face severe access-to-care challenges; further patient coverage losses would deepen these disparities and strain the state’s healthcare safety net.
New York’s Difficult Practice Environment
Compounding these pressures, New York consistently ranks among the worst states in the nation to practice medicine. Physicians in New York face:
- The highest medical liability costs in the country — exceeding the combined payouts of California and Florida.
- High office overhead expenses and administrative burdens.
- One of the nation’s heaviest tax and regulatory environments.
These factors make it increasingly difficult to attract and retain physicians, particularly in underserved areas.
A Call for Partnership and Reform
Given these developments, MSSNY urges the State Legislature and the Governor to take immediate action to improve New York’s practice environment. Efforts should focus on:
- Strengthening physician recruitment and retention.
- Reducing liability and administrative burdens.
- Ensuring adequate reimbursement and funding stability.
- Rejecting proposals that would further impede patient access to physician-led care.
Physicians across New York stand ready to partner with state policymakers to address these complex challenges. Together, we can design solutions that preserve patient access, sustain the physician workforce, and safeguard the delivery of high-quality care without imposing new barriers that compromise the health of New Yorkers.
 Health insurer–imposed administrative barriers continue to obstruct patient care delivery and intentionally delay fair payment to physicians. MSSNY will once again advocate for strong legislation and regulatory oversight to eliminate these abusive practices that undermine both patient access and physician sustainability.
Health insurer–imposed administrative barriers continue to obstruct patient care delivery and intentionally delay fair payment to physicians. MSSNY will once again advocate for strong legislation and regulatory oversight to eliminate these abusive practices that undermine both patient access and physician sustainability.
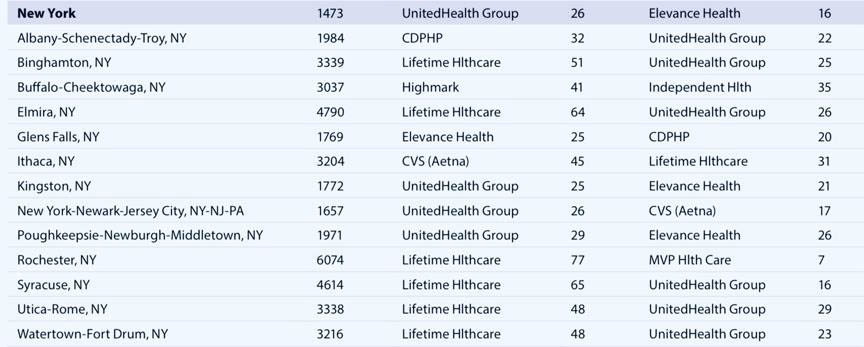
Insurers are able to impose these burdens because of their overwhelming market dominance across most regions of New York State. According to the 2024 AMA Competition Report, two large national companies, UnitedHealth and Elevance Health, are dominant players in nearly every regional market. Their market power forces most physicians to either accept unfavorable insurer terms or join large health systems simply to remain viable and continue caring for their communities.
Health Insurer Regional Market Domination
 Reducing Prior Authorization Burdens
Reducing Prior Authorization Burdens
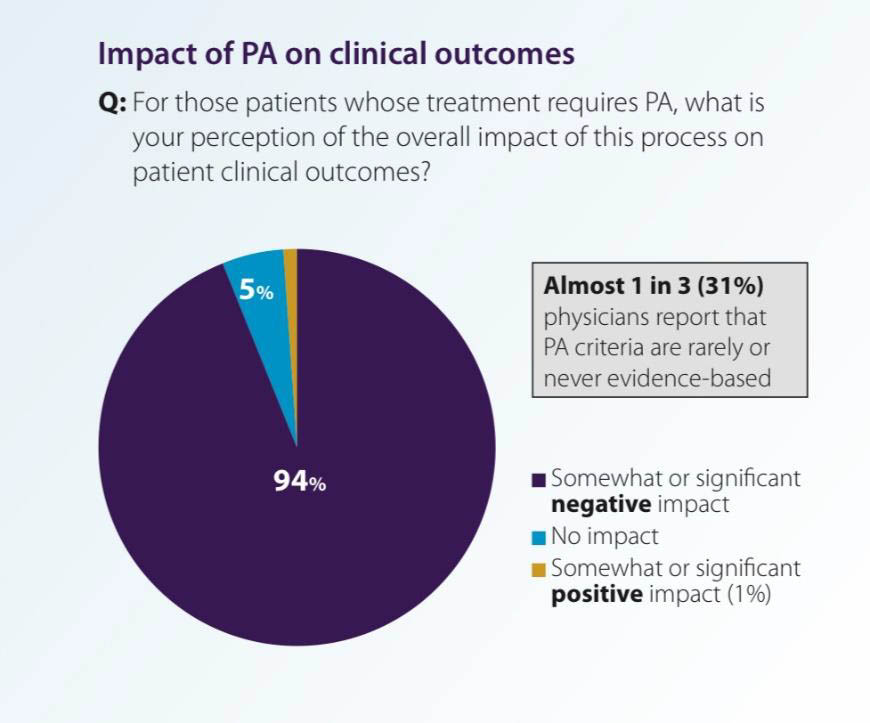
One way insurers exert this dominance is through overly complex and unnecessary prior authorization (PA) requirements. An AMA study released in February 2025 found that:
- 93% of physicians reported care delays due to PA requirements;
- 82% said these burdens led patients to abandon treatments;
- 94% reported negative clinical outcomes due to excessive PA; and
- 58% indicated that PA obstacles interfered with patients’ ability to work.
To address these problems, MSSNY continues to vigorously support legislation to reduce prior authorization hassles, including:
- Prohibiting repeat PAs for the same treatment and patient once an insurer has already granted authorization;
- Exempting physicians with a 90% or higher PA approval rate from future PA requirements for that treatment; and
- Ensuring prompt payment for delivering preauthorized services.
 Increasing Penalties for Payment Delays
Increasing Penalties for Payment Delays
Another widespread insurer abuse involves delaying or reducing payments, often through downcoding or unjustified denials. In 2024, enforcement of New York’s
Prompt Payment Law by the Department of Financial Services (DFS) resulted in $82 million in wrongfully withheld payments being returned to physicians and hospitals; in 2023, the amount exceeded $120 million.
While these enforcement actions are commendable, they also underscore that the 30-year-old Prompt Payment statute is no longer a sufficient deterrent. MSSNY will therefore advocate for legislation to significantly increase Prompt Payment penalties and to grant DFS and the Department of Health authority to impose additional sanctions on insurers engaging in systemic payment delays or excessive medical record requests that serve to obstruct timely payment.
 Limiting Abusive Insurer Audits
Limiting Abusive Insurer Audits
Insurers frequently exploit audits as a backdoor tactic to recoup payments long after claims were initially approved, circumventing prompt payment rules. Despite existing time limits, some insurers or their subcontractors allege “fraudulent billing” to evade these restrictions, intimidating physicians into costly repayments that can threaten practice viability.
MSSNY supports a number of important reforms to rein in these abusive audit demands, including:
- Limiting the lookback period for insurer recovery demands;
- Requiring greater transparency of what is being attempted to be recouped;
- Preventing offsets against future payments;
- Ensuring applicability of these rules to self-insured plans; and
- Requiring state review of attempts to bypass statutory time
Supporting Enhanced Insurance Coverage
MSSNY strongly supports policies that preserve affordable, comprehensive health coverage and limit excessive patient cost-sharing through coinsurance and deductibles. This includes continued federal ACA premium subsidies, legislation to require coverage for out-of-network care and enabling patients to assign payment directly to out-of-network physicians.
Protecting the Right to Appeal
MSSNY supports maintaining physicians’ right to appeal underpayments through the Independent Dispute Resolution (IDR) system, including within Medicaid Managed Care (MMC). This process is vital to ensuring patients have access to skilled specialty care, especially urgent surgical care in hospitals. Without access to IDR, physicians could be forced to accept unreasonably low Medicaid payments, discouraging specialists from providing essential on-call services and worsening hospital staffing shortages. Eliminating IDR access could also prompt MMC plans to drop physicians from their networks, further restricting patient access.
Expanding Early Intervention
MSSNY supports legislative initiatives to develop a comprehensive plan expanding access to Early Intervention services for children who require developmental support.
 Protecting Patient Access in Public Insurance Programs
Protecting Patient Access in Public Insurance Programs
Nearly 30% of New Yorkers rely on Medicaid, the Essential Plan, or CHIP for health coverage. MSSNY will advocate to safeguard patient enrollment, streamline access to community-based care, and protect federal funding for Medicaid payment increases included in the 2025–26 State Budget.
Despite these modest gains, New York’s Medicaid reimbursement rates remain among the lowest in the nation, discouraging physician participation. MSSNY will push for reforms allowing physicians to be reimbursed for treating patients dually enrolled in Medicare and Medicaid, a restriction that currently reduces access to care.
Low public program payment rates prevent many practices from covering basic costs, leading to reduced capacity or closure. Policymakers must ensure fair compensation to sustain independent physician practices, which offer cost-effective, community-based care and prevent further consolidation by hospital systems.
 Ensuring Fair Telehealth Payment
Ensuring Fair Telehealth Payment
Telehealth remains a vital mode of care delivery, improving patient convenience and access. MSSNY successfully advocated for payment parity legislation in 2022, ensuring commercial and Medicaid plans reimburse telehealth services at the same rate as in-person care. The law, renewed in 2024, is set to expire in 2026. MSSNY will continue to work with specialty societies to make parity permanent.
Revising New Payment Consent Requirements
The 2024–25 State Budget introduced a requirement for physicians to obtain separate patient consent for payment, after services are rendered. This conflicts with federal and state mandates requiring cost disclosures before treatment. The Department of Health has indicated it will not enforce this impractical rule, and MSSNY supports legislation to revise and align consent requirements with real-world medical practice.
Questions Regarding the New York Health Act
We recognize that the challenges of our current health care system, including pervasive insurance company abuses, have prompted some to advocate for the creation of a single payor health insurance plan for New York State. However, the “real world” challenges of such a system must be thoroughly analyzed before there is serious consideration of such an enactment. Any proposal for a state-run health plan must be subject to rigorous analysis before implementation. Critical questions include:
- Will a government payer replicate the same administrative hassles imposed by insurers?
- Will physician payments be fair, or mirror the inadequate rates under Medicare and Medicaid that already limit access?
- Most importantly, will patients receive timely, high-quality care without bureaucratic barriers?
MSSNY remains committed to reforms that expand access, reduce insurer abuses, and strengthen the physician–patient relationship, without jeopardizing care quality or physician independence.
New Yorkers depend on access to both their community-based physicians and a stable regional healthcare safety net. Yet, our already strained healthcare system faces growing financial pressure from recent federal cuts, pressures that are made far worse by New York’s outlier medical liability system. These excessive liability costs directly undermine hospitals and physicians’ ability to provide access to quality patient care.
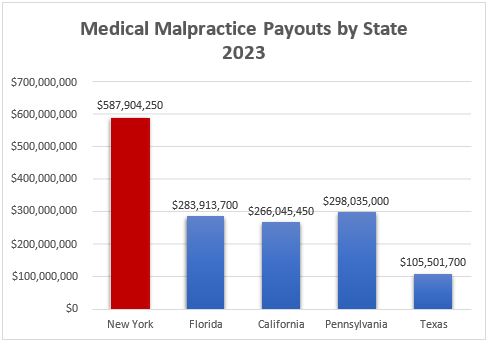
New York’s medical liability payouts are the highest in the nation. The state’s “tort tax” costs each household roughly $7,000, which affects affordability for all New Yorkers. This is one of the main reasons New York is one of the worst states in which to practice medicine.
 Despite the urgent need for reform, the Legislature has repeatedly advanced bills to inflate liability costs through expanded wrongful death awards (sometimes referred to as the “Grieving Families Act”). If enacted, this bill would necessitate premium increases of nearly 40%. Fortunately, Governor Hochul has vetoed these proposals, noting that they would raise insurance burdens for families and small businesses and impose untenable strain on already distressed healthcare institutions, particularly those in underserved communities. She also cautioned against the “significant unintended consequences” such legislation would create by threatening the financial viability of hospitals and community healthcare providers through steep increases in liability awards.
Despite the urgent need for reform, the Legislature has repeatedly advanced bills to inflate liability costs through expanded wrongful death awards (sometimes referred to as the “Grieving Families Act”). If enacted, this bill would necessitate premium increases of nearly 40%. Fortunately, Governor Hochul has vetoed these proposals, noting that they would raise insurance burdens for families and small businesses and impose untenable strain on already distressed healthcare institutions, particularly those in underserved communities. She also cautioned against the “significant unintended consequences” such legislation would create by threatening the financial viability of hospitals and community healthcare providers through steep increases in liability awards.
Nevertheless, in 2025, the Legislature again passed another one-sided version of the wrongful death expansion bill. MSSNY, along with many allied organizations, continues to urge lawmakers to reject piecemeal proposals and instead develop comprehensive liability reform that addresses costs, fairness, and access to care.
While many other states have passed laws to contain medical liability payouts and provide greater fairness in medical liability litigation, New York has not. As a result, our state’s medical liability payouts are double those of Pennsylvania, the next highest state, and exceed the combined totals of California and Florida. MSSNY urges the Governor to convene a healthcare liability reform task force of various healthcare stakeholders to craft a sustainable, systemwide plan to lower costs and protect access to care. See Malpractice Payouts by State.
MSSNY-Supported Measures to Reduce Liability Costs
- Strengthen Certificates of Merit: Require more detailed justification for filing malpractice suits. Two-thirds of claims result in no payment to plaintiffs yet cost millions in defense expenses.
- Require Peer Expert Witnesses: Expert witnesses should practice in the same specialty as the defendant
- Limit Excessive Non-Economic Damages: Adopt reasonable caps on non-economic damages, as over 30 other states have done.
- Create Alternative Dispute Resolution Systems: Establish medical courts or funds such as a Neurologically Impaired Infants Fund to handle claims more fairly.
- Modernize Court Judgment Interest Rates: Reduce the outdated 9% rate to a fair, market-based rate.
- Preserve Comprehensive Malpractice Coverage: Continue full funding for New York’s Excess Medical Malpractice Insurance Program, protecting 16,000 physicians from the state’s disproportionate liability MSSNY also opposes unfair cost-sharing mandates that would deter participation in this essential program. Until true liability reform is enacted, this protection remains critical to keeping physicians in New York.
Additional MSSNY Advocacy
- Oppose Attorney Fee Increases: Maintain consumer protections against excessive contingency fees in malpractice cases.
- Oppose Pre-Trial Cost-Sharing: Reject proposals requiring defendants to determine cost-sharing before trial outcomes.
- Oppose Pre-Judgment Interest Awards: Prevent interest accrual prior to final civil judgments, which unfairly increases total liability costs.
Strengthening Peer Review and Care Improvement
MSSNY supports strong protections for physician peer review discussions essential to improving patient safety and care quality. New York’s current laws, weakened further by the Siegel v. Snyder decision, allow trial lawyers to access confidential peer review statements, suppressing open dialogue. MSSNY urges enactment of legislation to restore full confidentiality to peer review proceedings, ensuring that physicians can engage candidly in quality improvement without fear of litigation exposure.
To ensure patients receive the highest quality care, MSSNY strongly supports efforts to preserve physician-led team care across New York State. This approach not only produces the best clinical outcomes but also aligns with patient preferences. A national survey found that 95% of patients believe it is important that a physician be involved in their diagnosis and treatment decisions.
Efforts to address physician shortages must focus on attracting and retaining physicians, rather than attempting to replace them. Key strategies include expanding the Doctors Across New York medical student loan repayment program, creating more clinical training opportunities for appropriately supervised international medical graduates
(IMGs), increasing inadequate Medicaid and other insurance reimbursement rates, and prohibiting non-compete clauses that disrupt continuity of care by restricting physicians’ ability to change practice settings.
The Value of Physician Oversight
Removing the crucial oversight and coordination provided by a trained physician can have significant adverse consequences for patients. Physicians play a central role in ordering and interpreting diagnostic tests, assessing the effectiveness of medications and treatments, and monitoring patients’ ongoing response to care. These functions are vital safeguards that ensure a patient’s unique clinical circumstances are fully considered and that potential complications or comorbidities are not overlooked.
The Importance of Training
The comprehensive education and clinical training required to become a physician are unmatched in scope and rigor. Physicians complete four years of medical school and an additional three to seven years of residency and fellowship training, accumulating 10,000–16,000 hours of clinical experience before practicing independently. This depth of education, which includes roughly 5,000 hours of medical school training, 4,000 internship hours, and 6,000–18,000 hours of specialty training, prepares physicians to deliver and coordinate complex medical care safely and effectively.
The Cost-Effectiveness of Physician-Led Care
Expanding non-physician scopes of practice is often promoted as a solution to workforce shortages, but the evidence shows otherwise. Studies demonstrate that independent non-physician practice increases costs and may compromise quality. For example, one analysis found that care provided exclusively by nurse practitioners (NPs) and physician assistants (PAs) was more expensive because these providers ordered more diagnostic tests and specialist referrals than physicians. Another study of NPs in Veterans Health Administration emergency departments found that unsupervised NP care increased patient length of stay by 11% and raised 30-day preventable hospitalizations by 20% compared to care by emergency physicians.
Legislative Priorities
 To help patients make informed decisions, MSSNY supports “Truth in Advertising” legislation requiring all healthcare providers to clearly identify their professional licensure in all settings and advertisements, especially when using the title “doctor.”
To help patients make informed decisions, MSSNY supports “Truth in Advertising” legislation requiring all healthcare providers to clearly identify their professional licensure in all settings and advertisements, especially when using the title “doctor.”
Legislation enacted in 2024 expanded PA flexibility to coordinate care and order certain services; this law should be carefully evaluated for its safety and effectiveness before any further expansion.
MSSNY opposes legislation that removes physician oversight in patient care, including proposals that would:
- Permit certified registered nurse anesthetists (CRNAs) to practice independently.
- Authorize independent practice for PAs or allow them to perform fluoroscopy without
- Expand nurse practitioner (NP) authority to provide care without collaboration with a physician in the same specialty.
- Allow podiatrists to perform ankle replacement surgery or treat patients up to the knee.
- Permit pharmacists to order or conduct laboratory tests without physician
- Grant psychologists prescribing
- Permit optometrists to perform surgical
Conversely, MSSNY supports allowing otolaryngologists to dispense hearing aids at fair market value — a logical step given that federal regulations now permit the over-the-counter sale of hearing aids. MSSNY also supports the ability of medical assistants to provide immunizations under physician supervision.
A Better Path Forward
New Yorkers deserve care that is either provided by or coordinated with a highly trained physician. Strengthening New York’s physician practice environment, rather than replacing physicians with non-physician providers, is the most effective and practical way to promote patient safety, expand access, and ensure the highest quality of care.
Providing Needed Patient Care Without Threat of Sanction
The Medical Society of the State of New York (MSSNY) maintains that physicians should be able to exercise independent clinical judgment when caring for patients. It supports legal protections for physicians who provide medical services that are lawful in New York, even if those services are restricted in other states (Policy 40.999).
One area that continues to receive close attention is reproductive health care. MSSNY supports legal measures to protect New York–licensed physicians who treat patients from New York or other states, either in person or via telemedicine, provided that such care complies with New York laws and regulations. MSSNY policy (5.990) supports legislation ensuring that providers of comprehensive women’s health services permitted under New York law are not subject to out-of-state prosecution or extradition. It also supports mechanisms allowing those sued in another state to provide such care in New York to seek legal recourse for interference with their protected rights.
MSSNY further maintains that oversight of reproductive health medications should remain under the authority of the U.S. Food and Drug Administration (FDA). It supports efforts to ensure continued access to mifepristone and misoprostol when appropriately prescribed and to preserve the FDA’s role as the primary regulator of these medications (Policy 5.989). MSSNY also supports increased access to emergency contraception, broader distribution options, and comprehensive sexual health education for adolescents.
Recognizing the importance of evidence-based medicine, MSSNY supports appropriate legal protections for physicians who provide gender-affirming care and opposes efforts to criminalize such care for minors (Policy 285.985).
End-of-Life Care
In 2025, both chambers of the New York State Legislature passed legislation that would allow mentally competent, terminally ill adults with a prognosis of six months or less to request from their physician a prescription for medication they may choose to self-administer to hasten death. The bill includes procedural safeguards and provides legal protections for physicians who comply with its provisions. At present, it is not yet known whether the Governor will sign the measure into law.
While ethical and moral considerations remain part of the public discussion, a majority of MSSNY’s House of Delegates expressed support for “medical aid in dying” legislation, provided that participation by physicians remains voluntary (Policy 95.964). This position was reaffirmed at the 2025 House of Delegates meeting.
MSSNY also advocates for several initiatives to improve end-of-life care, including:
- Establishing a statewide repository for Medical Orders for Life-Sustaining Treatment (MOLST)
- Ensuring appropriate reimbursement for physicians who provide end-of-life
- Expanding options for individuals seeking long-term care
MSSNY affirms that all patients should have access to high-quality end-of-life care, including hospice services.
MSSNY continues to advocate for universal access to recommended vaccinations, which have played a critical role in preventing disease and improving population health. Vaccination protects individuals and contributes to community-wide immunity.
In 2019, MSSNY supported legislation requiring all students attending public, private, or parochial schools to be immunized, except when medically contraindicated. While medical exemptions have increased in recent years, MSSNY maintains that medical contraindication should remain the only acceptable reason for exemption from school immunization requirements.
MSSNY supports the New York State Department of Health’s efforts to increase vaccination rates and encourages all health insurers to cover recommended immunizations without cost-sharing. It also supports legislation requiring schools in New York State and New York City to report immunization rates and exemptions to a centralized Department of Health database. Additionally, MSSNY advocates for universal reporting of adult immunizations to the New York State Immunization Information System (NYSIIS).
Substance Use Disorders
New York has achieved a substantial reduction in opioid prescribing, from over 9 million prescriptions in 2013 to
5.37 million in 2023, a decline of more than 40%. According to the CDC, New York now ranks among the states with the lowest opioid dispensing rates.
At the same time, additional regulations have introduced new administrative requirements for prescribers, including mandatory electronic prescribing, continuing medical education (CME) in pain management, limits on initial opioid prescriptions for acute pain, treatment plans for chronic use, and consideration of non-opioid alternatives.
The CDC’s 2022 Clinical Practice Guidelines emphasize evidence-based and patient-centered pain management. MSSNY has supported these principles through physician education, offering pain management CME since 2016 and a 2024 refresher course on the PMP Registry. The organization also supports expanded access to medication-assisted treatment (MAT), including methadone, and continued education for both physicians and patients on substance use disorder treatment options.
MSSNY advocates for seamless connection from New York’s Prescription Monitoring Program (PMP) to a physician’s electronic medical records (EMR). New York is one of the only states that maintains a system that does not integrate the PMP to an EMR. If implemented, this would further expand the use of the PMP registry and greatly reduce the administrative burdens to physicians and other care providers in accessing the PMP information.
Minimizing Community Health Impacts of Hospital Closures
Hospital closures or service reductions can limit access to care and increase pressure on nearby facilities. To help mitigate these effects, MSSNY’s House of Delegates adopted policy (150.959) encouraging meaningful local physician and patient participation in any proposal to close, downsize, or repurpose hospitals.
MSSNY supports legislation requiring advance public notice and community hearings before a hospital closure or significant service reduction, to promote transparency and ensure that community health needs are considered.
Health Equity
MSSNY has adopted a policy statement (285.986) recognizing that racism contributes to disparities in health outcomes and should be addressed as a public health issue. The organization is committed to advancing equity through its policies and programs.
Through its Committee on Health Equity, MSSNY seeks to:
- Increase understanding of how structural and social inequities, including racism, classism, sexism, ableism, ageism and xenophobia, affect health outcomes.
- Collaborate with partners such as the AMA, specialty societies, community organizations, and policymakers to address disparities affecting historically underserved populations.
- Promote education and equitable reimbursement for conditions that disproportionately impact under-resourced communities, such as diabetes, hypertension, and cancer.
Work to reduce disparities in outcomes such as maternal mortality, support diversity in the physician workforce, increase representation in medical education, and expand pipeline programs in rural and urban areas to address physician shortages.